
Get Paid What You're Owed, Without the Spreadsheet Chase
Owners, RCM leaders, and CFOs spend too much time stitching reports together to answer simple questions. Did we bill for all the care we delivered? Are we getting paid what's in our contracts? Why is this payer suddenly denying everything? Fuse pulls insurance checks, claims, adjudicated claims, and payer and patient payments into one place so the answers are already there.
SCHEDULE A DEMO
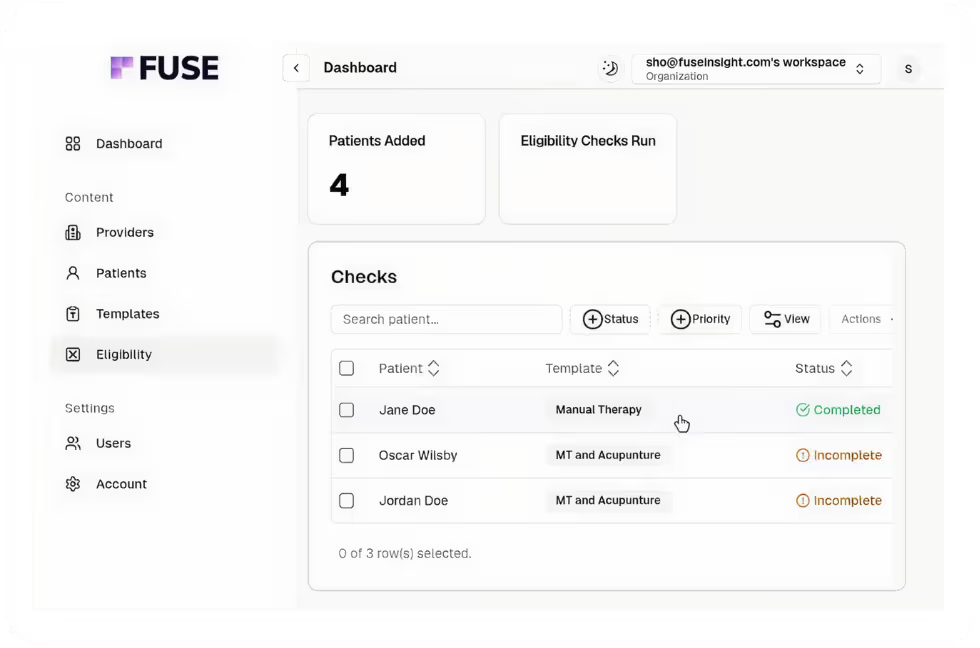








Stop Reconciling Spreadsheets From Different EMRs
Most groups end up with one EMR per site, one clearinghouse view, and a finance team that exports CSVs every Monday to glue it all together. By the time the numbers agree, the questions have moved on.
Aged A/R, contract underpayment, and denial spikes are decisions waiting on a reconciliation that should have been automatic.
Your Financial
Command Center
Fuse ties insurance checks, claims, adjudicated claims, and payments to the same encounter, payer, and site. That is what turns four disconnected feeds into clear answers about cash, denials, contracts, and A/R.
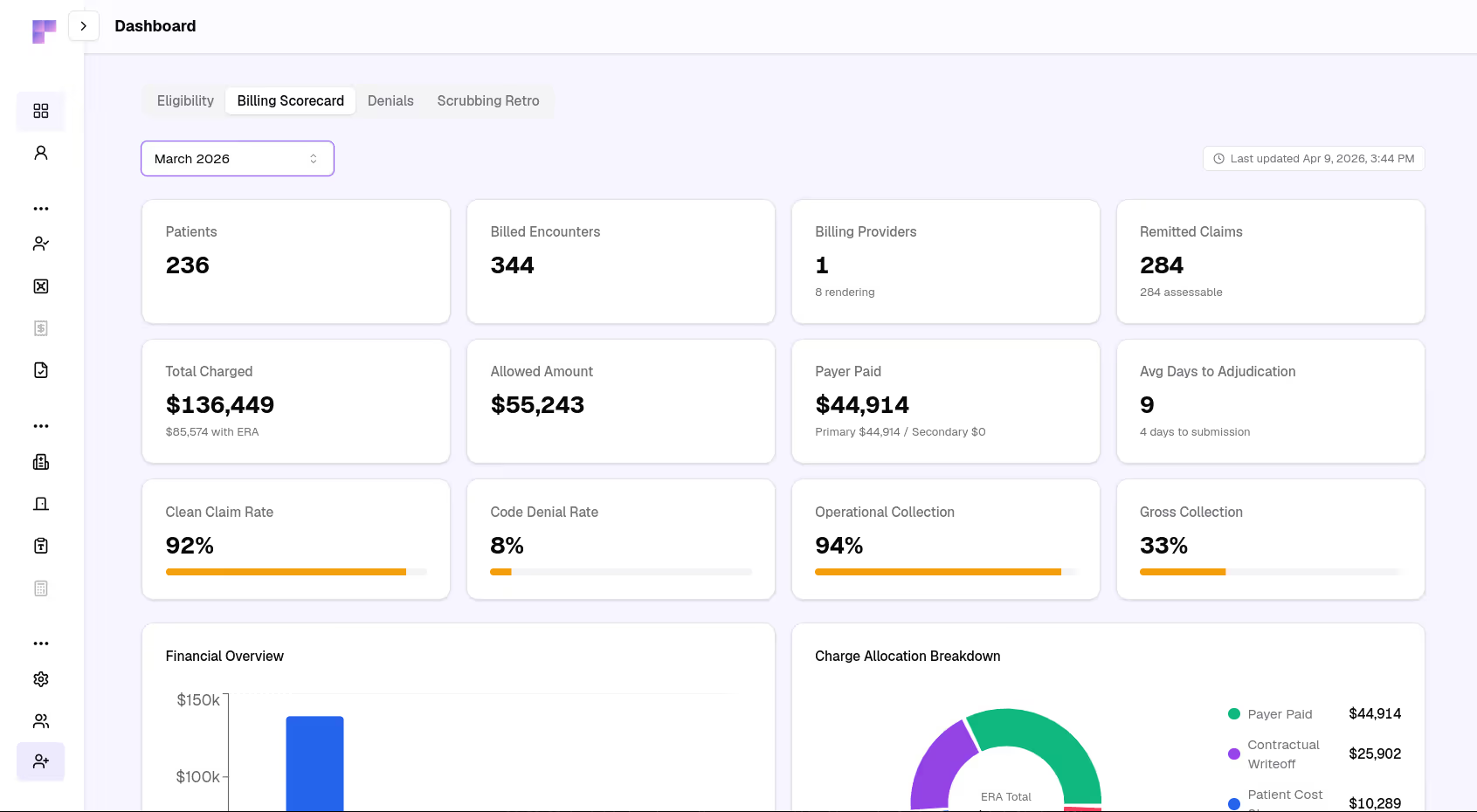
Eligibility and benefits checks capture what a payer represented going into the visit: active coverage, cost-sharing, and authorization signals. They are a starting point, not proof of payment. Revenue intelligence keeps that pre-service expectation linked to the claim and the payment so leadership can see when reality diverged and why.
Adjudicated claims and the remittance behind them are the ground truth: what was allowed, what was paid, what was adjusted, and what the patient owes. That is where revenue intelligence answers whether insurance paid everything you billed, whether a new denial is a one-off or a pattern, and whether underpayments are drifting from your contracts.
The expensive gaps live between systems: visits that never became a claim, claims sitting unworked between submission and denial, and denials that quietly age past timely filing. Putting eligibility, claims, denials, and payments on one timeline makes those gaps visible the week they happen, not the quarter after.
Patient payments, payer payments, and contracted rates only mean something next to each other. Compared together, you can see whether each payer is paying what they agreed to, where patient responsibility is being collected, and where dollars are slipping out of either side of the ledger.
One View Across Every Site
For groups operating across multiple locations, Fuse defines A/R, denials, cash, and contract metrics once and applies them consistently across every site and billing entity. Numbers roll up at the group level and drill down to a single location, payer, or claim, so leadership and finance work from the same view and the monthly reporting cycle stops eating analyst time.
- Compare cash, denials, and aged A/R by location
- Reconcile what hit the bank against what was billed
- See which payers are behaving differently across sites
- Give boards and investors a defensible revenue story


Intelligence Built for the People Running the Practice
Operating leaders should not have to guess at the health of their revenue. Fuse turns the four feeds that already flow through your practice, insurance checks, claims, adjudicated claims, and payments, into a single picture of where money is earned, where it is sitting, and where it is leaking. Aged A/R becomes a worklist instead of a number on a slide. Unbilled care surfaces while the encounter is still fresh, not in a year-end clean-up. Underpayments show up as patterns by payer and procedure code, with a contract benchmark next to them so the conversation with the payer starts with evidence.
For owners, that means seeing margin and cash by site, payer, and service line without rebuilding a spreadsheet every month. For RCM leaders, it means denial spikes, policy shifts, and stalled claims are visible the week they happen, with the staff workload prioritized by deadline and dollar value. For CFOs, it is a defensible revenue narrative for the board: what was billed, what was paid, what is still recoverable, and which payers are quietly shifting the rules.


Stop Reconciling in Spreadsheets
Your team already has the data. What is missing is one place that turns it into answers leadership can act on. Schedule a demo to see Fuse revenue intelligence in your numbers.
SCHEDULE A DEMOFAQs
What is Fuse revenue intelligence?
It is the layer of Fuse that turns your operational data into financial answers. We connect insurance checks, claims, adjudicated claims, and payer and patient payments to the same encounter, payer, and site, then expose that as scorecards and worklists for leadership and RCM teams.
What data does Fuse pull together?
Eligibility and benefits responses, outcomes from automated payer phone calls, claim submission events, adjudicated claims and remittance, payer payments, and patient payments. Where you have payer contracts loaded, we use those too so paid amounts can be benchmarked against expected rates.
Does Fuse work across multiple sites and EMRs?
Yes. Fuse normalizes data from each location into one set of definitions so A/R, denials, cash, and contract metrics mean the same thing across sites and billing entities. You can roll metrics up at the group level and drill down to a single location, payer, or claim.
How is this different from a clearinghouse or EMR report?
Clearinghouses and EMRs are good at the slice they own. Neither connects benefits expectations, claim outcomes, payments, and contracts in one place. Fuse sits across all of them so leadership can explain variance instead of stitching exports together.
How does Fuse spot underpayments and denial spikes?
Underpayments are detected by comparing paid amounts to your contracted rates by procedure code and payer plan and surfacing variance over a configurable threshold. Denial spikes are detected by clustering denial and remark codes by payer, plan, and procedure over time and alerting when a code is suddenly outside its baseline.
How does Fuse help with aged A/R and denial deadlines?
Open balances are bucketed by age, payer, and site, and tied to the last claim event so your team knows what is still actionable. Denials are ranked by timely-filing and appeal windows so the work that pays off the most, and is closest to expiring, is at the top of the list.
How current is the data?
Fuse is built to reflect new eligibility, claim, denial, and payment activity as it arrives, so leadership views match the latest payer behavior rather than a monthly static export. The exact cadence depends on how your EMR and clearinghouse hand data off.
Is Fuse HIPAA compliant?
Yes. Fuse is HIPAA compliant and SOC 2 Type II certified. Revenue intelligence runs on the same security and privacy controls as the rest of the platform. Visit Fuse's security page for policies and audits.


