
Stop Losing Revenue to Preventable Claim Denials
Registration and eligibility errors are the number one cause of claim denials, accounting for 24% of all rejections according to the Optum 2024 Revenue Cycle Denials Index. Half of these are non-recoverable. No appeals path, no rework opportunity. The revenue is permanently lost.
These are front-end errors: coordination of benefits problems, benefit maximum issues, plan coverage gaps, and patient eligibility mismatches. Fuse automates eligibility verification at the CPT code level to catch these issues before services are rendered, protecting revenue that would otherwise be written off.

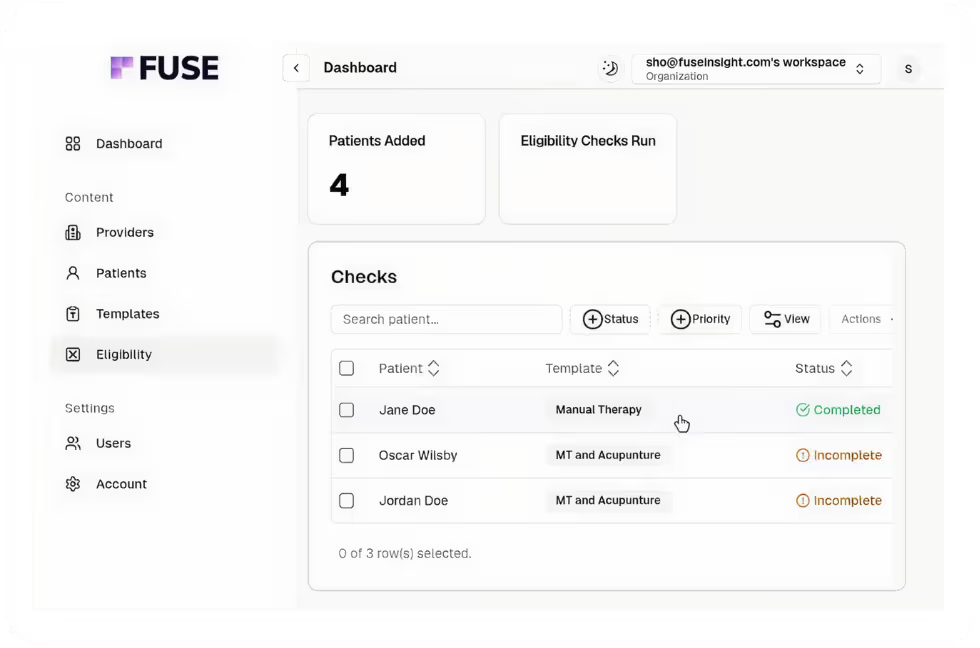








Registration and Eligibility Errors: The Leading Cause of Rejected Claims
Registration and eligibility issues have been the top denial category since 2016. The average denial rate across U.S. hospitals has climbed to 12%, up from 9% in 2016, and eligibility errors now represent 24% of all denials, up from 22% the prior year. Front-end issues overall account for 44% of all claim rejections.
The real cost is not just the volume of rejections. It is the fact that 50% of registration and eligibility rejections are non-recoverable. The root causes tell the story: coordination of benefits problems account for 50% of eligibility rejections, benefit maximum issues for 27%, plan coverage gaps for 17%, and patient eligibility mismatches for 6%. Each of these is a front-end problem that could have been caught before the claim was ever submitted.
Why Basic Eligibility Checks
Miss Critical Coverage Issues
A basic eligibility check confirms that a patient has active insurance. It does not confirm whether the specific procedure you plan to bill is covered, whether the patient has hit a benefit maximum, or whether another payer should be billed first. That gap between general eligibility and procedure-level coverage is where most non-recoverable rejections originate.
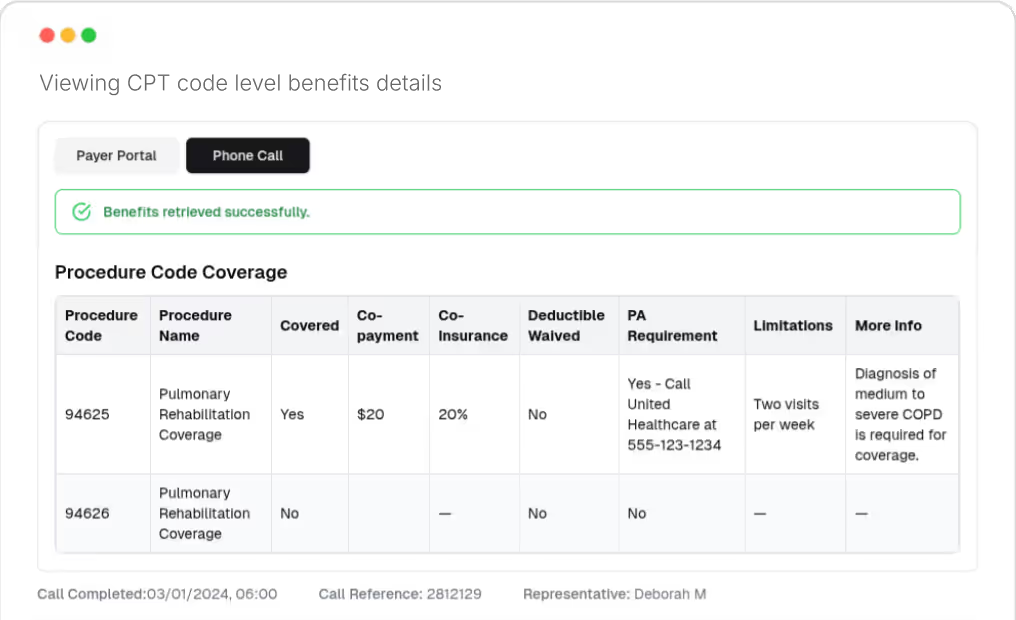
Coordination of benefits issues account for 50% of all eligibility-related rejections. Many patients carry coverage through multiple payers, and billing the wrong primary insurer triggers an automatic denial. Payer portals do not reliably surface COB information, so the problem often goes undetected until the claim comes back rejected. By that point, timely filing deadlines with the correct payer may have passed, turning a fixable error into a permanent write-off.
Benefit maximum issues cause 27% of eligibility rejections, and plan coverage gaps cause another 17%. Detecting these requires knowing what the patient has already used against their plan and whether the specific procedure is covered under their benefits. A general eligibility check confirms active coverage but does not reveal that a patient has exhausted their visit limit for physical therapy or that their plan excludes the specific CPT code you intend to bill.
Basic eligibility confirms a patient has insurance. CPT-level verification confirms whether that insurance actually covers the procedure you plan to perform, what the patient will owe, and whether prior authorization is required. Without this level of detail, your practice renders services, submits a claim, and discovers the coverage gap only when the rejection arrives. With 84% of all denials classified as potentially avoidable, the opportunity to prevent revenue loss sits squarely at the front end of the revenue cycle.
How Fuse Catches Coverage Issues Before You Bill
Fuse verifies insurance at the CPT code level, checking coverage for the specific procedures you plan to bill. The system confirms exact copays, coinsurance, and deductible amounts per procedure, identifies prior authorization requirements before scheduling, and confirms network status through payer portals, direct payer phone calls, and adjudicated claims data at the payer plan level.
When half of eligibility rejections cannot be recovered, prevention protects revenue that would otherwise be permanently lost. Verifying at the CPT level before the appointment means coordination of benefits problems, benefit maximums, and plan coverage gaps are caught while there is still time to address them.
- Digital patient intake captures insurance before arrival
- CPT-level verification confirms procedure-specific coverage
- Prior auth requirements identified during eligibility check
- Network status confirmed via portal checks and payer calls
- Exact patient responsibility calculated upfront


The Revenue Math: What Prevention Is Worth
Consider what these numbers mean for a typical practice. If your average denial rate is 12% and registration/eligibility errors account for 24% of those denials, nearly 3% of all your claims are being rejected for eligibility reasons alone. Half of those rejections are non-recoverable. That is 1.5% of your total claim volume turning into permanent revenue loss, every month, with no path to recovery.
The Optum data also shows that 84% of all denials are potentially avoidable. CPT-level verification targets the single largest denial category at the exact point in the revenue cycle where prevention is still possible: before services are rendered. That makes front-end eligibility verification the highest-ROI investment in the revenue cycle. Every denial you prevent is revenue you keep, and every non-recoverable rejection you avoid is money that would have been written off permanently.


Protect Your Revenue from Permanent Write-Offs
With 24% of rejections from eligibility errors and half non-recoverable, front-end verification is the highest-ROI revenue cycle investment. Fuse combines automated insurance verification, CPT-level benefits checks, and adjudicated claims data to catch coverage issues before you bill. Less rejection volume means lower administrative costs. Fewer non-recoverable rejections means revenue stays in your practice and improves patient collections, with denial trends and recoverable A/R surfaced in revenue intelligence for RCM and finance leaders.
Schedule a demo to see how Fuse helps specialty practices prevent eligibility-related rejections before services are rendered.
FAQs
What percentage of claim denials are caused by eligibility errors?
Fuse automates eligibility verification to address the single largest denial category: registration and eligibility errors, which account for 24% of all claim denials according to the Optum 2024 Revenue Cycle Denials Index. This category has held the top position since 2016 and has trended upward from 22% in recent years. Front-end issues overall, which include eligibility errors, account for 44% of all claim rejections.
What percentage of eligibility-related rejections are non-recoverable?
Fuse's eligibility verification protects against the approximately 50% of eligibility-related rejections that are non-recoverable, meaning there is no appeals path and the revenue is permanently lost. Unlike coding errors or clinical documentation issues that can often be corrected and resubmitted, many eligibility rejections result from coverage gaps, coordination of benefits problems or benefit maximums that cannot be resolved after services have been rendered.
Why do coordination of benefits issues cause so many denials?
Fuse's CPT-level verification catches coordination of benefits issues before services are rendered. These issues cause 50% of all eligibility-related rejections because many patients have coverage through multiple payers and billing the wrong primary insurer results in an automatic denial. Payer portals do not reliably surface COB (coordination of benefits) information, so practices often discover the problem only after the claim is rejected. By that point, timely filing deadlines with the correct payer may have passed, making the denial non-recoverable.
What is CPT-level eligibility verification?
Fuse's CPT-level eligibility verification confirms insurance coverage for specific procedure codes rather than just checking whether a patient has active insurance. This includes verifying exact copays, coinsurance, deductible application, prior authorization requirements and visit limits for each planned procedure. Fuse performs this verification through payer portals, direct payer calls and adjudicated claims data at the payer plan level.
How often should insurance eligibility be verified?
Fuse verifies insurance eligibility before every scheduled appointment, ideally at the time of scheduling and again 24 to 48 hours before the visit. Patient coverage can change between appointments due to job changes, plan switches or benefit exhaustion. Verifying at both points catches coverage gaps early enough to resolve them or reschedule, preventing services from being rendered under invalid or insufficient coverage.
How does Fuse catch coverage issues before claims are submitted?
Fuse verifies insurance at the CPT code level, checking coverage for the specific procedures the practice plans to bill. Fuse confirms exact copays, coinsurance and deductible amounts per procedure, identifies prior authorization requirements before scheduling and confirms network status through payer portals, direct payer phone calls and adjudicated claims data at the payer plan level. With 84% of all denials classified as potentially avoidable, Fuse's front-end CPT-level verification is the highest-ROI investment in the revenue cycle.


