
Improve Collections with Accurate Patient Fee Estimates
Patient collection rates dropped to 34.4% for commercially insured patients in 2024, down from 37.6% the year before. On average, providers collect just 24% of patient billings after insurance. The gap between what patients owe and what practices actually collect keeps growing, and most of it traces back to the same root causes: inaccurate estimates, surprise bills, and manual follow-up that never happens.
Fuse helps practices reduce bad debt by automating insurance verification, generating precise patient cost estimates, and automating reminders and billing using AI. When patients know what they owe before they walk in, they pay faster and your staff spends less time chasing balances.









Why Bad Debt Keeps Growing for Healthcare Practices
The patient portion of healthcare payments has risen 30% since 2000. More patients are on high-deductible health plans, which means greater out-of-pocket costs and a larger share of every bill landing on the patient. Hospital bad debt climbed 40% compared to 2022, with another 10% increase in 2025 alone.
When practices lack transparent pricing and effective patient payment collection strategies, administrators spend more time chasing payments than delivering care. Squeezed margins limit investment in technology and staffing, creating a cycle where collections get worse and bad debt keeps climbing. Breaking that cycle starts with giving patients accurate cost information before their appointment, not after the bill goes out.
How Accurate Patient Fee Estimates
Improve Your Collection Rate
Most billing problems start before the bill is ever sent. When patients receive an estimate that does not match their final charge, trust erodes and payments stall. Fuse generates fee estimates using real-time, CPT-level insurance data combined with adjudicated claims history, so the number your patient sees at scheduling is the number they actually owe.
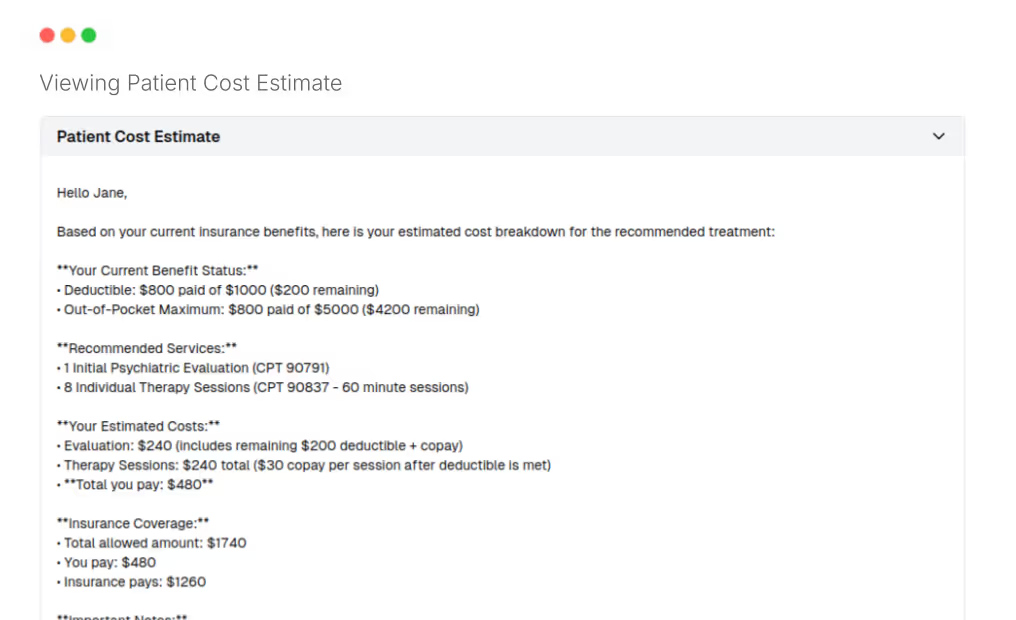
In a 2026 survey, 81% of patients said accurate estimates helped them prepare to pay for healthcare costs. Practices that use price estimation tools experience faster, more predictable cash flow because patients can budget ahead of time. When there are no surprises on the bill, disputes drop, payment timelines shorten, and your front desk spends less time fielding calls about unexpected charges.
Most estimates are built on general eligibility data, which confirms that a patient has active coverage but misses procedure-specific deductibles, coinsurance tiers, and prior authorization requirements. The result is a ballpark number that may not reflect what the patient actually owes. When the final bill arrives higher than expected, patients delay payment or dispute the charge, driving up bad debt and admin costs.
Fuse verifies insurance benefits at the CPT code level by checking payer portals, placing direct payer phone calls, and analyzing adjudicated claims data at the payer plan level. Over time, the system remembers results for each payer and plan combination, making every subsequent verification faster and more accurate. That means confirming the exact copay, coinsurance, deductible application, and authorization requirements for each procedure you plan to bill. The result is a precise estimate, not a range, that gives both your practice and your patients the confidence to plan ahead.
How Patient Collection Automation Reduces Bad Debt
Most EMR systems were not built for patient collections. Invoices go out with inaccurate amounts, there are no automated nudges, and staff are left manually following up on outstanding balances. The result: without structured payment prompts, practices collect just 7% of patient balances compared to 77% with them.
Fuse uses verified insurance data and your EMR records to calculate accurate bills and automate patient communications. From the initial estimate through final payment, patients receive clear, consistent information about what they owe and how to pay. Practices using pre-payment systems see 20% higher collection rates, and your staff is freed from the manual follow-up that consumes their day.
- Insurance verification and CPT-level benefits checks
- Patient fee estimate generation from real-time data
- Automated invoicing, reminders, and payment follow-up


Real Results from Transparent Pricing
The data is clear: pricing transparency drives measurable improvements in patient collections. One health system saw a 27% increase in upfront payments, totaling over $2 million in annual revenue. Hospitals using self-service estimate portals have increased collection rates by up to 133%. Digital payment tools reduce the billing cycle by 35% and boost collections by 28%.
Across the industry, practices that combine accurate estimates with automated billing see a 15 to 40% improvement in patient responsibility collection rates. These are not theoretical gains. They come from giving patients real numbers before their appointment and making it easy to pay.


Start Improving Patient Collections with Fuse
Fuse connects the entire collections workflow: automated insurance verification, granular CPT-level benefits data, accurate patient cost estimates, and automated billing and reminders, all wired into the revenue intelligence layer your leadership team uses to track cash and denials. Your staff gets time back, your patients get clarity, and your practice collects more of what it earns.
Schedule a demo to see how Fuse reduces bad debt and improves patient collections through automation.
FAQs
Why is patient bad debt growing for healthcare practices?
Fuse helps practices reduce bad debt caused by inaccurate estimates, surprise bills and manual follow-up that never happens. The patient portion of healthcare payments has risen 30% since 2000, and hospital bad debt climbed 40% compared to 2022 with another 10% increase in 2025 alone. More patients are on high-deductible health plans, which means greater out-of-pocket costs and a larger share of every bill landing on the patient.
What is a good medical billing collection rate for patient responsibility?
Fuse helps practices reduce bad debt and improve patient collections. A good medical billing collection rate for patient responsibility is 80% or higher, though top-performing practices aim for 90% or above. In reality, most practices fall well short of that benchmark. In 2024, the average collection rate for commercially insured patients dropped to 34.4%, down from 37.6% the year before. Closing that gap requires accurate estimates, transparent pricing and automated follow-up.
How do patient fee estimates help improve collections for healthcare practices?
Fuse generates fee estimates using real-time, CPT-level insurance data combined with adjudicated claims history, so the number a patient sees at scheduling is the number they actually owe. In a 2026 Experian Health survey, 81% of patients said accurate estimates helped them budget for healthcare costs. Practices that provide upfront pricing see fewer billing disputes, faster payments and lower bad debt because patients are not caught off guard by unexpected charges.
How does insurance verification at the CPT code level improve collections?
Fuse's CPT-level insurance verification improves collections by producing accurate patient cost estimates based on the exact procedures you plan to bill, rather than general eligibility data. Standard eligibility checks confirm that a patient has active coverage but miss procedure-specific copays, coinsurance tiers and deductible application. Fuse verifies benefits at the CPT code level through payer portals, direct payer calls and adjudicated claims data at the payer plan level, giving your staff the precise data needed to quote a real number before the appointment.
Can upfront pricing transparency really increase payment collection rates?
Yes, Fuse connects accurate estimates with automated billing and reminders to deliver upfront pricing transparency. Practices that combine accurate estimates with automated billing see a 15 to 40% improvement in patient responsibility collection rates. Hospitals using self-service estimate portals have increased collections by up to 133%, according to Experian. Practices that implement structured payment prompts collect 77% of patient balances compared to just 7% without them. Transparent pricing builds trust, reduces billing disputes and gives patients the information they need to pay on time.
How does Fuse automate patient invoicing, reminders and collections?
Fuse automates patient invoicing by combining verified insurance data with your EMR records to generate accurate bills, then sends automated payment reminders to patients on a scheduled cadence. Fuse calculates patient responsibility using CPT-level benefits data, creates clear invoices that match the pre-service estimate and follows up with patients who have outstanding balances. This reduces manual staff follow-up and helps practices collect more without adding administrative burden.


