
Patient Billing That Doesn't Create More Work
Most patient billing issues start before the bill is even sent. Inaccurate charges from missed coverage details, wrong copay amounts, or outdated insurance information create a cascade of problems: patients call to dispute, staff spend hours explaining charges, and payments stall.
The typical EMR sends one text with the bill and provides no visibility into whether patients paid, how many times they have been contacted, or where the balance stands. Fuse addresses billing accuracy at the source by automating insurance verification before services are rendered, so patient responsibility is calculated correctly from the start.

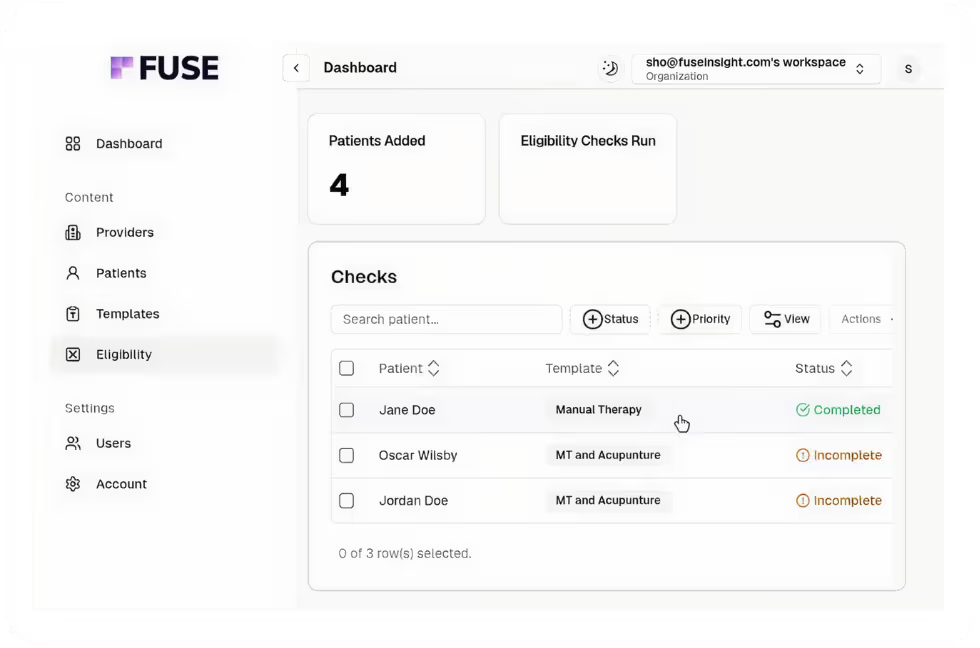








Why Patients Call About Their Bills
Patients don't call because they don't want to pay. They call because something looks wrong: a charge they didn't expect, a copay that doesn't match what they were told, or services they thought were covered. These calls consume significant staff time and often reveal the same root cause: incomplete or inaccurate eligibility information at the time of service.
When the front desk couldn't confirm exact copays, coinsurance, or coverage limitations, the patient received a bill that didn't match their expectations. Now your team is spending 15 to 30 minutes per call explaining charges that could have been communicated upfront.
The Hidden Cost of
Send and Hope Billing
Most EMR systems send a single bill notification with no follow-up automation and no visibility into patient response. There is no tracking for how many times a patient has been contacted, whether they have viewed the bill, or where the balance stands in the collection cycle. Staff have no dashboard showing which patients need follow-up and which payments are at risk.
Most EMRs send a single notification and leave it at that. There is no way to see whether the patient opened the bill, whether they started a payment, or whether the message even reached them. Your billing team is working blind, with no data to prioritize follow-up or identify at-risk balances before they age into collection problems.
Without automated follow-up or a clear view of outstanding balances, unpaid bills sit untouched for weeks or months. By the time staff realize a patient hasn't paid, the window for easy resolution has closed. What could have been a quick payment conversation at the point of service becomes a collections problem that costs more to resolve than the original balance.
Every billing call that results from inaccurate charges takes 15 to 30 minutes of staff time. These are not complex clinical questions. They are patients asking why their copay is different than expected or why a service they thought was covered appears on their bill. Each call traces back to the same root cause: eligibility information that was incomplete when the charge was created.
Accurate Bills Start with Accurate Eligibility
Fuse approaches billing differently: fix the accuracy problem before the bill exists. Automated eligibility verification at the CPT code level confirms exact patient responsibility before the appointment. Patients know their copay, coinsurance, and deductible amounts upfront because Fuse verified coverage through payer portals, direct payer calls, and adjudicated claims data at the payer plan level.
When the bill arrives, it matches what the patient was told. No surprises. No disputes. No calls asking why the charge is different than expected. This upstream accuracy eliminates the most common source of billing friction and accelerates time to payment.
- Exact copays and coinsurance confirmed per CPT code before service
- Prior authorization requirements verified to prevent claim rejections
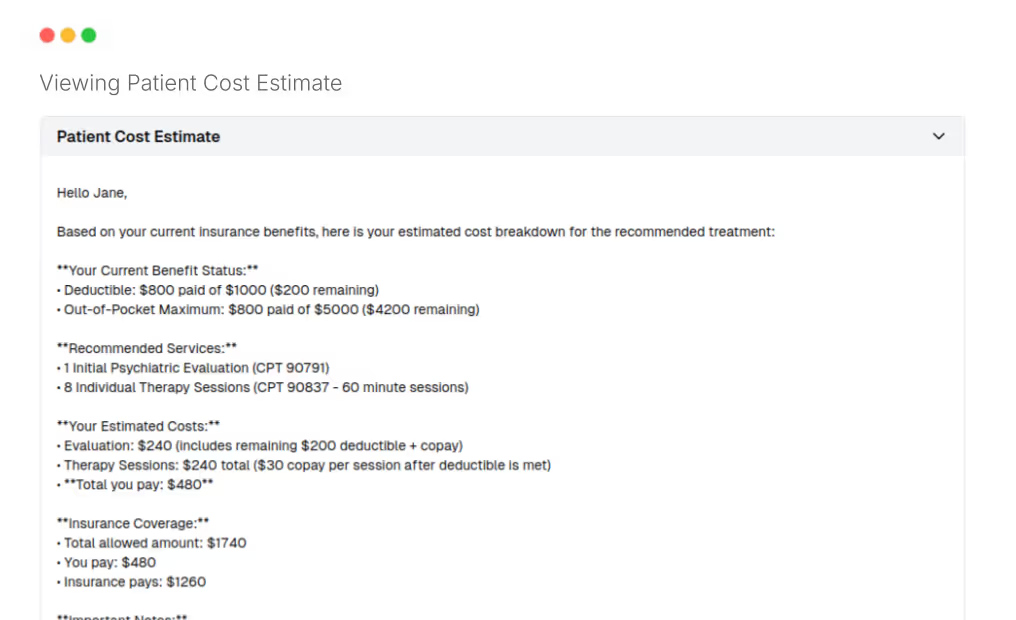
- Patient cost estimate provided before the appointment


When Bills Are Accurate, Collections Follow
When patient responsibility is calculated correctly from the start, the downstream billing process runs smoother. Patients receive accurate cost estimates before their appointment, so the bill is not a surprise. Staff spend less time fielding billing questions and more time on higher-value work.
Collections improve because patients are more likely to pay bills they understand and expected. Practices that provide upfront pricing transparency see fewer disputes, faster payments, and lower bad debt. The pattern is consistent: accurate eligibility data in, accurate bills out, faster collections as a result.


Reduce Billing Calls, Accelerate Collections
When patient responsibility is calculated correctly from the start, bills are accurate, patients pay faster, and your staff spends less time on the phone. Fuse automates insurance verification at the CPT code level so every bill reflects what the patient actually owes.
Schedule a demo to see how Fuse's eligibility verification creates accurate patient bills that collect faster with fewer disputes.
FAQs
Why do patients dispute medical bills?
Patients dispute bills when charges don't match their expectations, typically because copays, coinsurance, or coverage details weren't accurately communicated before their visit. The root cause is usually incomplete eligibility verification that failed to capture exact patient responsibility at the CPT code level. When patients are told one amount and billed another, they call to dispute the difference.
How does eligibility verification reduce billing disputes?
CPT-level eligibility verification reduces billing disputes by confirming exact copays, coinsurance, and deductible amounts for each planned procedure before the appointment. This allows staff to give patients accurate cost estimates upfront. When the bill matches what the patient was told to expect, disputes and billing-related calls decrease significantly.
What causes inaccurate patient charges?
Inaccurate patient charges typically result from incomplete insurance verification: wrong copay amounts from checking general eligibility rather than procedure-specific benefits, or outdated insurance information that was never re-verified. Basic portal checks often miss procedure-specific details, while CPT-level verification with payer calls confirms exact patient responsibility before charges become billing errors.
How can practices reduce patient billing calls?
The most effective way to reduce billing calls is to ensure accuracy before the bill is sent. Automated eligibility verification that confirms exact patient responsibility at the CPT code level eliminates the most common reasons patients call: unexpected charges, copay discrepancies, and coverage confusion. When bills match patient expectations, call volume decreases.
What is the connection between eligibility verification and patient collections?
Eligibility verification directly impacts collections because accurate bills collect faster. When patients receive bills that match their expectations, they are more likely to pay promptly. Verification also identifies patients with high deductibles or limited coverage before the appointment, allowing practices to collect patient responsibility upfront or establish payment arrangements before services are rendered.


