
Know Exactly What's Covered Before the Appointment
Patients call your front desk with two questions: "Is this covered?" and "What will I owe?" Basic eligibility checks can't answer either. They confirm a patient has active insurance, not whether their plan covers the specific procedure you're about to perform or what the patient will actually pay.
Fuse verifies insurance at the CPT code level. That means checking coverage for the exact procedures you plan to bill, confirming copays, coinsurance, deductible application, visit limits, and prior authorization requirements before services are rendered. Your staff gets the details they need. Your patients get real answers.

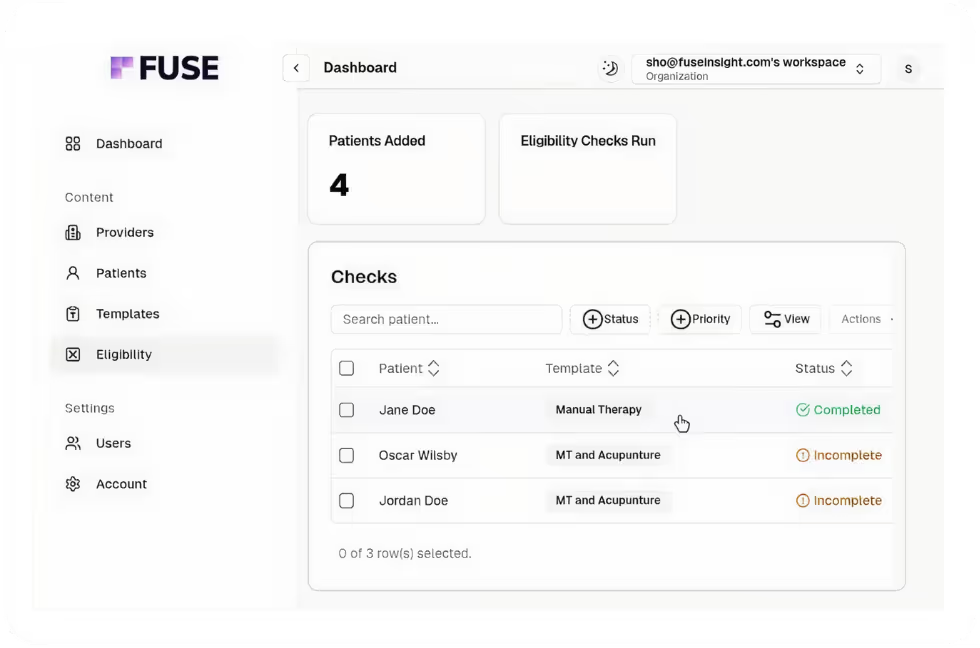









Why General Eligibility Checks Fall Short
Portals like Availity, pVerify, and Office Ally confirm that a patient has active coverage. They might show a specialist visit copay or a list of service type codes. But they won't tell you the exact copay for an initial psychiatric evaluation versus a follow-up therapy session, or whether a specific procedure code is covered at all. In many cases, they show multiple copay amounts without clarifying which one applies to your service.
That leaves your staff with three options: guess, call the payer and wait on hold, or bill and hope for the best. The result is predictable. Patients get surprise bills they weren't expecting. Your front desk fields calls asking why the charge doesn't match what they were told. Claims get denied for coverage issues that could have been caught before the appointment.
What CPT-Level
Verification Reveals
For each procedure code you plan to bill, Fuse confirms whether the service is covered, the exact patient responsibility, and any requirements that could delay or deny the claim. This is the information your staff needs to answer coverage questions confidently at scheduling or check-in, not after the bill goes out.
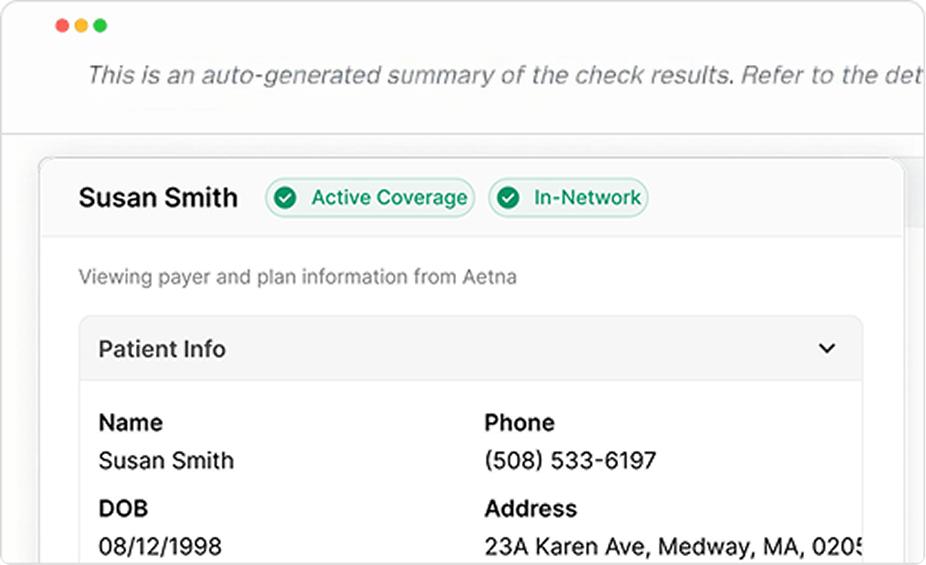
This level of detail answers the questions patients actually ask. When a new patient calls to schedule an initial evaluation, your staff can tell them exactly what their plan covers and what they'll owe. No callbacks, no guesswork, no "we'll let you know after we bill.
This level of detail answers the questions patients actually ask. When a new patient calls to schedule an initial evaluation, your staff can tell them exactly what their plan covers and what they'll owe. No callbacks, no guesswork, no "we'll let you know after we bill.
This level of detail answers the questions patients actually ask. When a new patient calls to schedule an initial evaluation, your staff can tell them exactly what their plan covers and what they'll owe. No callbacks, no guesswork, no "we'll let you know after we bill.

Automated Portal Checks and Payer Calls
Portals provide baseline coverage data, but they rarely include procedure-specific details. The specifics, like whether a particular CPT code requires prior authorization, what the exact copay is, or how the payer classifies your billing provider, typically require a phone call.
Fuse automates both. We check payer portals for general eligibility and then place direct payer calls to fill in the gaps. The results are combined into a single, clear summary. Your staff gets complete benefits information without toggling between portals, dialing payer lines, or reconciling conflicting data.
Payer portal checks for baseline coverage dataDirect payer phone calls for CPT-specific benefitsIn-network/out-of-network status confirmation




